The three types of Ultra Violet radiation are classified according to their wavelength.
They differ in their biological activity and the extent to which they can penetrate the skin. The shorter the wavelength, the more harmful the UV radiation. However, shorter wavelength UV radiation is less able to penetrate the skin.
The Ultra Violet region covers the wavelength range 100-400 nm and is divided into three bands:
- UVA (315-400 nm)
- UVB (280-315 nm)
- UVC (100-280 nm).
Short-wavelength UVC is the most damaging type of UV radiation. However, it is completely filtered by the atmosphere and does not reach the earth’s surface.
Medium-wavelength UVB is very biologically active but cannot penetrate beyond the superficial skin layers. It is responsible for delayed tanning and burning; in addition to these short-term effects it enhances skin ageing and significantly promotes the development of skin cancer. Most solar UVB is filtered by the atmosphere.
The relatively long-wavelength UVA accounts for approximately 95 per cent of the UV radiation reaching the Earth’s surface. It can penetrate into the deeper layers of the skin and is responsible for the immediate tanning effect. Furthermore, it also contributes to skin ageing and wrinkling. For a long time it was thought that UVA could not cause any lasting damage. Recent studies strongly suggest that it may also enhance the development of skin cancers.
Treatment: One is prevention and avoid sun light when it is out the strongest in ultra-violet rays 12pm to 3pm and always use sunscreen.
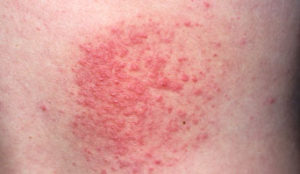
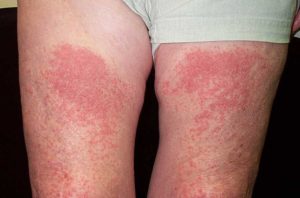
Polymorphic light eruption (PLE) is the most common form of immunologically mediated photosensitivity dermatoses. Exposure to sunlight in spring or summer results in an irritable rash that resolves within a few days, providing further exposure is avoided.
The following treatments may reduce the severity of PLE:
- Topical corticosteroid creams to relieve symptoms
- Short course of oral steroids, eg to cover a summer holiday
- Hydroxychloroquine
- Phototherapy: UVB narrowband UVB, or PUVA for several weeks in early spring.
Are there any other health issues related to UV radiation?
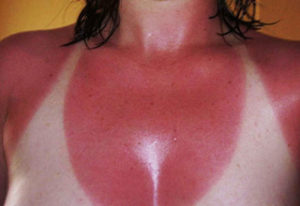
In addition to cancer, exposure to UV rays can cause other health problems. UV rays, either from the sun or from artificial sources like tanning beds, can cause sunburn. In some people, exposure to UV rays can cause a rash or a type of allergic reaction. Exposure to UV rays can also cause premature aging of the skin and signs of sun damage such as liver spots, actinic keratosis, and solar elastosis.
UV rays can also cause eye problems. They can cause the cornea (on the front of the eye) to become inflamed or burned. They can also lead to the formation of cataracts (clouding of the lens of the eye) and pterygium (tissue growth on the surface of the eye), both of which can impair vision.
Exposure to UV rays can also weaken the immune system, so that the body has a harder time fending off infections. This can lead to problems such as reactivation of herpes triggered by exposure to the sun or other sources of UV rays. It can also cause vaccines to be less effective.
Some medications can make you more sensitive to UV radiation, making you more likely to get sunburned. Certain medical conditions can be made worse by UV radiation.
About UV rays and vitamin D
Doctors are learning that vitamin D has many health benefits. It might even help lower the risk for some cancers. Your skin makes vitamin D naturally when it is exposed to UV rays from the sun. How much vitamin D you make depends on many things, including how old you are, how dark your skin is, and how strong the sunlight is where you live.
At this time, doctors aren’t sure what the optimal level of vitamin D is. A lot of research is being done in this area. Whenever possible, it’s better to get vitamin D from your diet or vitamin supplements rather than from exposure to UV rays because dietary sources and vitamin supplements do not increase skin cancer risk, and are typically more reliable ways to get the amount you need.
Remember tips about UV rays for men and women:
Men, especially those with lighter skin, are more likely than anybody else to get skin cancer, including melanoma—the deadliest kind of skin cancer.
When you think about sun protection, you might think about a day at the beach. But over your lifetime, you get sun exposure doing everyday things like biking, working, running, or even mowing the lawn. Sun exposure is the main source of ultraviolet (UV) rays, which can cause skin cancer. And UV exposure adds up over time, increasing your risk of developing skin cancer.
Men tend to get more sun exposure than women. Men spend more time outside over their lifetimes than women, and they’re more likely to work outdoors than women. Women’s personal care products, like moisturizer and makeup, often contain sunscreen, while many products for men don’t.
About one-third of U.S. adults get sunburned each year. Sunburn, which can increase your risk of getting skin cancer, is common among white men, young adults, and men who tan indoors. When outside on a sunny day for more than an hour, only about 14% of men use sunscreen on both their face and other exposed skin.
Seek shade, especially during midday hours. This includes 10 am to 4 pm, March through October, and 9 am to 3 pm, November through February. Umbrellas, trees, or other shelters can provide relief from the sun.
Wear a long-sleeved shirt and pants or a long skirt for additional protection when possible. If that’s not practical, try wearing a T-shirt or a beach cover-up.
Apply a thick layer of broad spectrum sunscreen with an SPF of 15 or higher at least 15 minutes before going outside, even on cloudy or overcast days. Reapply sunscreen at least every 2 hours and after swimming, sweating, or toweling off.
Indoor and outdoor tanning often begin in the teen years and continue into adulthood. Don’t wait to teach your children about the dangers of tanning. Children may be more receptive than teens, so start the conversation early, before they start outdoor tanning or indoor tanning. For example, you can Discourage tanning, even if it’s just before one event like prom. UV exposure adds up over time. Every time you tan, you increase your risk of getting skin cancer. Help preteens and teens understand the dangers of tanning so they can make healthy choices.
There is no such thing as a safety tan!!!!