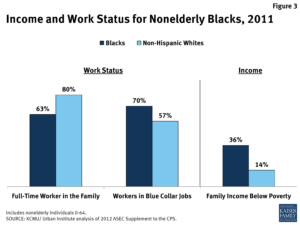
The majority of Americans black or white under 67.5 have to work to have medical coverage (unless under disability), if not the majority of Americans would be rich.
Health care disparities heighten disease differences between African-Americans and white Americans.
- African-Americans are three times more likely to die of asthma than white Americans.
- Diabetes is 60% more common in black Americans than in white Americans. Blacks are up to 2.5 times more likely to suffer a limb amputation and up to 5.6 times more likely to suffer kidney disease than other people with diabetes.
- Deaths from lung scarring — sarcoidosis — are 16 times more common among blacks than among whites. The disease recently killed former NFL star Reggie White at age 43.
- Despite lower tobacco exposure, black men are 50% more likely than white men to get lung cancer.
- Strokes kill 4 times more 35- to 54-year-old black Americans than white Americans. Blacks have nearly twice the first-time stroke risk of whites.
- Blacks develop high blood pressure earlier in life — and with much higher blood pressure levels — than whites. Nearly 42% of black men and more than 45% of black women aged 20 and older have high blood pressure.
- Cancer treatment is equally successful for all races. Yet black men have a 40% higher cancer death rate than white men. African-American women have a 20% higher cancer death rate than white women.
Why?
Factor 1 – Genes definitely play a role. So does the environment in which people live, socioeconomic status, says Clyde W. Yancy, MD, associate dean of clinical affairs and medical director for heart failure/transplantation at the University of Texas Southwestern Medical Center.
Living in a low socioeconomic environment puts you at risk to eating fast foods or deli food (especially in the cities) and increasing, over long term eating fast foods, causing disease (DM, Obesity, Heart Disease and could go on).
Factor 2 – Another reason is that a higher percentage of black Americans than white Americans live close to toxic waste dumps — and to the factories that produce this waste.
Addressing socioeconomic groups first, Dr. Yancy says that all humans have the same physiology, are vulnerable to the same illnesses, and respond to the same medicines. Naturally, diseases and responses to treatment do vary from person to person. But, he says, there are unique issues that affect black Americans.
Like Yancy, LeRoy M. Graham Jr., MD, says the time is ripe for Americans to come to grips with these issues. Graham, a pediatric lung expert, serves on the American Lung Association’s board of directors, is associate clinical professor of pediatrics at Morehouse School of Medicine in Atlanta, and serves as staff physician for Children’s Healthcare of Atlanta.
“I just think we as physicians need to get more impassioned,” Graham tells WebMD. “There are health disparities. There are things that may have more sinister origins in institutionalized racism. But we as doctors need to spend more time recognizing these disparities and addressing them — together with our patients — on a very individual level.”
A 2005 report from the American Lung Association shows that black Americans suffer far more lung disease than white Americans do.
Some of the findings:
- Black Americans have more asthma than any racial or ethnic group in America. And blacks are 3 times more likely to die of asthma than whites.
- Black Americans are 3 times more likely to suffer sarcoidosis than white Americans. The lung-scarring disease is 16 times more deadly for blacks than for whites.
- Black American children are 3 times as likely as white American children to have sleep apnea.
- Black American babies die of sudden infant death syndrome (SIDS) 2.5 times as often as white American babies.
- Black American men are 50% more likely to get lung cancer than white American men. For starters this race is highier overall than caucasians in smoking in the U.S.A.
- Black Americans are half as likely to get flu and pneumonia vaccinations as white Americans.
“The environment is involved, and there is potential genetic susceptibility — but we also have to talk about the fact that African-Americans’ social and economic status lags behind that of Caucasians,” Graham says. “And low socioeconomic status is linked to more disease.”
Of course these 2 factors put you at risk for disease, but you want to live in a better environment do your research. Some may say it due to blacks being treated poorly or the word “racism”. Is this the case, No not at all. You need the facts why you blacks are highier in living in a toxic or low socioeconomic group. One, that is where they can afford and decide to live their. Two is because they feel they can not or they decide not to move due to personal reasons like lack to apply self to get in a better environment (whether it be due to fear, lack of knowing their success in the move/challenge so they don’t want to take the chance or not wanting change and decide to stay in that toxic or low socio-economic area. No one puts a magnum 45 to anyone’s head telling them they have to stay in these areas. In America you can live where you want. So its up to the individual with the family having the will to make the move in their life to be less exposed to areas poor for you health. Its up to them to research areas less expensive or better enviroment exposure areas in America; no one else is going to do that for them or any one else. Than there are those that simply don’t mind living in areas like toxic or low socioeconomic exposed but many don’t understand that thinking. The risk is that individual and their family put themselves at risk for a higher chance of getting these diseases like lung cancer, heart disease, etc… Make the move and get out of those places and live a better quality of life for you and all in your family. Its all up to you to make the move. Keep in mind disease is not just environmental related. You need to look at all factors like genetic, the diet you are on, how active you are; its not just one factor in most cases. You have to take a holistic approach on seeing what diseases you could be exposed to and why. Don’t wait till symptoms start finding out its possibly too late. Think PREVENTION over treatment. Its your life and up to you!
Part II tomorrow