Continuation of Other Types of Glaucoma:
Normal-Tension Glaucoma (NTG)
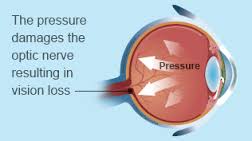
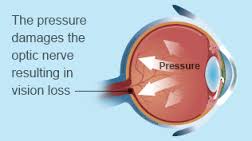
Also called low-tension or normal-pressure glaucoma. In normal-tension glaucoma the optic nerve is damaged even though the eye pressure is not very high. We still don’t know why some people’s optic nerves are damaged even though they have almost normal pressure levels.
Congenital Glaucoma
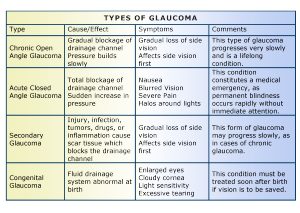
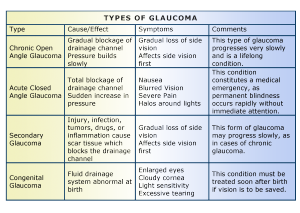
This type of glaucoma occurs in babies when there is incorrect or incomplete development of the eye’s drainage canals during the prenatal period. This is a rare condition that may be inherited. When uncomplicated, microsurgery can often correct the structural defects. Other cases are treated with medication and surgery.
Secondary Glaucomas
Sometimes glaucoma is caused by another medical condition — this is called secondary glaucoma.
Neovascular glaucoma
Treatments: Medicines, laser treatment, surgery
Neovascular glaucoma happens when the eye makes extra blood vessels that cover the part of your eye where fluid would normally drain. It’s usually caused by another medical condition, like diabetes or high blood pressure.
If you have neovascular glaucoma, you may notice:
- Pain or redness in your eye
- Vision loss
This type of glaucoma can be hard to treat. Doctors need to treat the underlying cause (like diabetes or high blood pressure) and use glaucoma treatments to lower the eye pressure that results from it.
Pigmentary glaucoma
Treatments: Medicines, laser treatment, surgery
Pigment dispersion syndrome happens when the pigment (color) from your iris (the colored part of your eye) flakes off. The loose pigment may block fluid from draining out of your eye, which can increase your eye pressure and cause pigmentary glaucoma.
Young, white men who are near-sighted are more likely to have pigment dispersion syndrome than others. If you have this condition, you may have blurry vision or see rainbow-colored rings around lights, especially when you exercise.
Doctors can treat pigmentary glaucoma by lowering eye pressure, but there currently isn’t a way to prevent pigment from detaching from the iris.
Exfoliation glaucoma
Treatments: Medicines, laser treatment, surgery
Exfoliation glaucoma (sometimes called pseudoexfoliation) is a type of open-angle glaucoma that happens in some people with exfoliation syndrome, a condition that causes extra material to detach from parts of the eye and block fluid from draining.
Recent research shows that genetics may play a role in exfoliation glaucoma. You are at higher risk if someone else in your family has exfoliation glaucoma.
This type of glaucoma can progress faster than primary open-angle glaucoma, and often causes higher eye pressure. This means that it’s especially important for people who are at risk to get eye exams regularly.
Uveitic glaucoma
Treatments: Medicines, surgery
Uveitic glaucoma can happen in people who have uveitis, a condition that causes inflammation (irritation and swelling) in the eye. About 2 in 10 people with uveitis will develop uveitic glaucoma.
Experts aren’t sure how uveitis causes uveitic glaucoma, but they think that it may happen because uveitis can cause inflammation and scar tissue in the middle of the eye. This may damage or block the part of the eye where fluid drains out, causing high eye pressure and leading to uveitic glaucoma.
In some cases, the medicines that treat uveitis may also cause uveitic glaucoma, or make it worse. This is because corticosteroid medicines may cause increased eye pressure as a side effect.
The KEY is take the steps to help PREVENT Glaucoma:
These self-care steps can help you detect glaucoma in its early stages, which is important in preventing vision loss or slowing its progress.
- Get regular dilated eye examinations. Regular comprehensive eye exams can help detect glaucoma in its early stages, before significant damage occurs. As a general rule, the American Academy of Ophthalmology recommends having a comprehensive eye exam every five to 10 years if you’re under 40 years old; every two to four years if you’re 40 to 54 years old; every one to three years if you’re 55 to 64 years old; and every one to two years if you’re older than 65. If you’re at risk of glaucoma, you’ll need more frequent screening. Ask your doctor to recommend the right screening schedule for you.
- Know your family’s eye health history. Glaucoma tends to run in families. If you’re at increased risk, you may need more frequent screening.
- Exercise safely. Regular, moderate exercise may help prevent glaucoma by reducing eye pressure. Talk with your doctor about an appropriate exercise program.
- Take prescribed eyedrops regularly. Glaucoma eyedrops can significantly reduce the risk that high eye pressure will progress to glaucoma. To be effective, eyedrops prescribed by your doctor need to be used regularly even if you have no symptoms.
- Wear eye protection. Serious eye injuries can lead to glaucoma. Wear eye protection when using power tools or playing high-speed racket sports in enclosed courts.