
Hall of Fame pitcher Tom Seaver, the star of the Miracle Mets 1969 World Series championship team, was diagnosed with dementia at age 74.
His family made the announcement Thursday through the Hall and said Seaver has retired from public life. He will continue to work at Seaver Vineyards, founded by the retired player and wife Nancy in 2002 on 116 acres at Diamond Mountain in the Calistoga region of California.
Seaver was diagnosed with Lyme disease in 1991, and it reoccurred in 2012 and led to Bell’s Palsy and memory loss, the New York Daily News reported in 2013.
Know this, Lyme disease also has the unique ability to bypass the body’s blood-brain barrier, a barrier which typically prevents foreign invaders from affecting the brain, allowing the disease to enter the nervous system accounting for Lyme’s many complex neurological symptoms. Antibiotic treatment protocols alone do not account for this invasion of the body’s nervous system through the blood-brain barrier and therefore are not likely to have lasting results. To effectively treat chronic Lyme disease, antibiotics need to also move past the blood-brain barrier.
Lyme related neurological symptoms are destructive and life-changing.
The struggle to find the right diagnosis is extremely draining for patients who are already facing depression, brain fog, memory loss, tremors, and other crippling symptoms.
Can this lead to Alzheimer’s disease or make it come quicker??
Art Shamsky, who hit .300 with 14 home runs that season for the Mets, details some of the health issues of other teammates as well, among other things, in “After the Miracle,” Newsday reported last week, March 6 on Fox News Channel.
Shamsky, 77, wrote that Seaver suffers from short-term memory loss that could stem from Lyme disease. Seaver, 74, apparently told Shamsky he contracted the disease in 1991 when he lived in Connecticut.
Bud Harrelson, another key player on the championship team, which defeated the Baltimore Orioles in the World Series, four games to one, had reportedly been making visits to Seaver regularly and told some members of the team to be prepared when they re-connected with the three-time Cy Young award winner.
“He can forget things that happened just a few minutes before,” Harrelson told Shamsky, according to Newsday. “And he repeats himself a lot. But when he gets his rest, he still has a lot of energy.”
Harrelson, 74, is having his own health struggles. The former Mets shortstop was diagnosed with Alzheimer’s disease in 2016. He opened up to CBS New York after 2016 and told the station he immediately stopped driving.


Overview of Dementia and many people can get it anywhere!
Dementia isn’t a specific disease. Instead, dementia describes a group of symptoms affecting memory, thinking and social abilities severely enough to interfere with daily functioning.
Though dementia generally involves memory loss, memory loss has different causes. So memory loss alone doesn’t mean you have dementia. So seeing a specialist who is a MD in Dementia is the expert to go to.
Alzheimer’s disease is the most common cause of a progressive dementia in older adults, but there are a number of causes of dementia. Depending on the cause, some dementia symptoms can be reversed.
Symptoms
Dementia symptoms vary depending on the cause, but common signs and symptoms include:
Cognitive changes
- Memory loss, which is usually noticed by a spouse or someone else
- Difficulty communicating or finding words
- Difficulty reasoning or problem-solving
- Difficulty handling complex tasks
- Difficulty with planning and organizing
- Difficulty with coordination and motor functions
- Confusion and disorientation
Psychological changes
- Personality changes
- Depression
- Anxiety
- Inappropriate behavior
- Paranoia
- Agitation
- Hallucinations
When to see a doctor
See a doctor if you or a loved one has memory problems or other dementia symptoms. Some treatable medical conditions can cause dementia symptoms, so it’s important to determine the underlying cause.
Causes
Dementia involves damage of nerve cells in the brain, which can occur in several areas of the brain. Dementia affects people differently, depending on the area of the brain affected.
Dementias are often grouped by what they have in common, such as the part of the brain that’s affected or whether they worsen over time (progressive dementias). Some dementias, such as those caused by a reaction to medications or vitamin deficiencies, might improve with treatment.
Progressive dementias
Types of dementias that progress and aren’t reversible include:
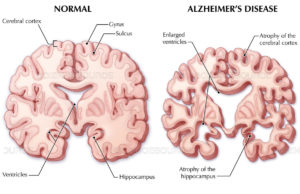
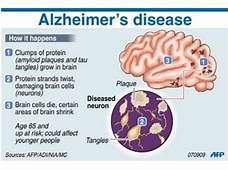
- Alzheimer’s disease. In people age 65 and older, Alzheimer’s disease is the most common cause of dementia.Although the cause of Alzheimer’s disease isn’t known, plaques and tangles are often found in the brains of people with Alzheimer’s. Plaques are clumps of a protein called beta-amyloid, and tangles are fibrous tangles made up of tau protein.Certain genetic factors might make it more likely that people will develop Alzheimer’s.
- Vascular dementia. This second most common type of dementia occurs as a result of damage to the vessels that supply blood to your brain. Blood vessel problems can be caused by stroke or other blood vessel conditions.
- Lewy body dementia. Lewy bodies are abnormal clumps of protein that have been found in the brains of people with Lewy body dementia, Alzheimer’s disease and Parkinson’s disease. This is one of the more common types of progressive dementia.
- Frontotemporal dementia. This is a group of diseases characterized by the breakdown (degeneration) of nerve cells in the frontal and temporal lobes of the brain, the areas generally associated with personality, behavior and language.As with other dementias, the cause isn’t known.
- Mixed dementia. Autopsy studies of the brains of people 80 and older who had dementia indicate that many had a combination of Alzheimer’s disease, vascular dementia and Lewy body dementia. Studies are ongoing to determine how having mixed dementia affects symptoms and treatments.
Other disorders linked to dementia
- Huntington’s disease. Caused by a genetic mutation, this disease causes certain nerve cells in your brain and spinal cord to waste away. Signs and symptoms, including a severe decline in thinking (cognitive) skills usually appear around age 30 or 40.
- Traumatic brain injury. This condition is caused by repetitive head trauma, such as experienced by boxers, football players or soldiers.Depending on the part of the brain that’s injured, this condition can cause dementia signs and symptoms, such as depression, explosiveness, memory loss, uncoordinated movement and impaired speech, as well as slow movement, tremors and rigidity (parkinsonism). Symptoms might not appear until years after the trauma.
- Creutzfeldt-Jakob disease. This rare brain disorder usually occurs in people without known risk factors. This condition might be due to an abnormal form of a protein. Creutzfeldt-Jakob disease can be inherited or caused by exposure to diseased brain or nervous system tissue.Signs and symptoms of this fatal condition usually appear around age 60.
- Parkinson’s disease. Many people with Parkinson’s disease eventually develop dementia symptoms (Parkinson’s disease dementia).
Dementia-like conditions that can be reversed
Some causes of dementia or dementia-like symptoms can be reversed with treatment. They include:
- Infections and immune disorders. Dementia-like symptoms can result from fever or other side effects of your body’s attempt to fight off an infection. Conditions such as multiple sclerosis that result from the body’s immune system attacking nerve cells also can cause dementia.
- Metabolic problems and endocrine abnormalities. People with thyroid problems, low blood sugar (hypoglycemia), too little or too much sodium or calcium, or an impaired ability to absorb vitamin B-12 can develop dementia-like symptoms or other personality changes.
- Nutritional deficiencies. Not drinking enough liquids (dehydration); not getting enough thiamin (vitamin B-1), which is common in people with chronic alcoholism; and not getting enough vitamins B-6 and B-12 in your diet can cause dementia-like symptoms.
- Reactions to medications. A reaction to a medication or an interaction of several medications can cause dementia-like symptoms.
- Subdural hematomas. Bleeding between the surface of the brain and the covering over the brain, which is common in the elderly after a fall, can cause symptoms similar to dementia.
- Poisoning. Exposure to heavy metals, such as lead, and other poisons, such as pesticides, as well as alcohol abuse or recreational drug use can lead to symptoms of dementia. Symptoms might resolve with treatment.
- Brain tumors. Rarely, dementia can result from damage caused by a brain tumor.
- Anoxia. This condition, also called hypoxia, occurs when organ tissues aren’t getting enough oxygen. Anoxia can occur due to severe asthma, heart attack, carbon monoxide poisoning or other causes.
- Normal-pressure hydrocephalus. This condition, which is caused by enlarged ventricles in the brain, can cause walking problems, urinary difficulty and memory loss.
Risk factors
Many factors can eventually lead to dementia. Some factors, such as age, can’t be changed. Others can be addressed to reduce your risk.
Risk factors that can’t be changed
- Age. The risk rises as you age, especially after age 65. However, dementia isn’t a normal part of aging, and dementia can occur in younger people.
- Family history. Having a family history of dementia puts you at greater risk of developing the condition. However, many people with a family history never develop symptoms, and many people without a family history do. Tests to determine whether you have certain genetic mutations are available.
- Down syndrome. By middle age, many people with Down syndrome develop early-onset Alzheimer’s disease.
- Mild cognitive impairment. This involves difficulties with memory but without loss of daily function. It puts people at higher risk of dementia.
Risk factors you can change
You might be able to control the following risk factors of dementia.
- Heavy alcohol use. If you drink large amounts of alcohol, you might have a higher risk of dementia. Some studies, however, have shown that moderate amounts of alcohol might have a protective effect.
- Cardiovascular risk factors. These include high blood pressure (hypertension), high cholesterol, buildup of fats in your artery walls (atherosclerosis) and obesity.
- Depression. Although not yet well-understood, late-life depression might indicate the development of dementia.
- Diabetes. If you have diabetes, you might have an increased risk of dementia, especially if it’s poorly controlled.
- Smoking. Smoking might increase your risk of developing dementia and blood vessel (vascular) diseases.
- Sleep apnea. People who snore and have episodes where they frequently stop breathing while asleep may have reversible memory loss.
Complications
Dementia can affect many body systems and, therefore, the ability to function. Dementia can lead to:
- Inadequate nutrition. Many people with dementia eventually reduce or stop their intake of nutrients. Ultimately, they may be unable to chew and swallow.
- Pneumonia. Difficulty swallowing increases the risk of choking or aspirating food into the lungs, which can block breathing and cause pneumonia.
- Inability to perform self-care tasks. As dementia progresses, it can interfere with bathing, dressing, brushing hair or teeth, using the toilet independently and taking medications accurately.
- Personal safety challenges. Some day-to-day situations can present safety issues for people with dementia, including driving, cooking and walking alone.
- Death. Late-stage dementia results in coma and death, often from infection.
Prevention
There’s no sure way to prevent dementia, but there are steps you can take that might help in slowing down the process of the disease. More research is needed, but it might be beneficial to do the following:
- Keep your mind active. Mentally stimulating activities, such as reading, solving puzzles and playing word games, and memory training might delay the onset of dementia and decrease its effects.
- Be physically and socially active. Physical activity and social interaction might delay the onset of dementia and reduce its symptoms. Move more and aim for 150 minutes of exercise a week.
- Quit smoking. Some studies have shown smoking in middle age and beyond may increase your risk of dementia and blood vessel (vascular) conditions. Quitting smoking might reduce your risk and will improve your health.
- Get enough vitamin D. Research suggests that people with low levels of vitamin D in their blood are more likely to develop Alzheimer’s disease and other forms of dementia. You can get vitamin D through certain foods, supplements and sun exposure.More study is needed before an increase in vitamin D intake is recommended for preventing dementia, but it’s a good idea to make sure you get adequate vitamin D.
- Lower your blood pressure. High blood pressure might lead to a higher risk of some types of dementia. More research is needed to determine whether treating high blood pressure may reduce the risk of dementia.
- Maintain a healthy diet. Eating a healthy diet is important for many reasons, but a diet such as the Mediterranean diet — rich in fruits, vegetables, whole grains and omega-3 fatty acids, commonly found in certain fish and nuts — might promote health and lower your risk of developing dementia.